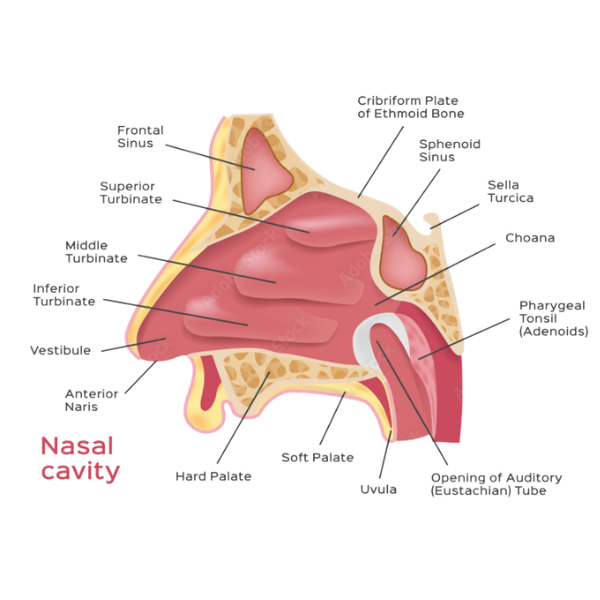
The Hidden Risk in Plain Sight: The Nasal Vestibule
Healthcare-associated infections (HAIs) remain one of the most persistent and costly challenges in modern medicine. Despite advances in sterilization and perioperative protocols, one major source of infection often goes under-addressed: the patient’s own nasal cavity.
The anterior nares (nasal vestibule) are a well-documented reservoir for pathogens, particularly Staphylococcus aureus, including MRSA.1 Studies consistently show that nasal carriers are at significantly higher risk of developing surgical site infections (SSIs) due to endogenous transfer of bacteria during or after procedures.2
This is the foundation of nasal decolonization—a preventive strategy designed to reduce microbial burden before it can cause harm.
From Optional to Essential: The Rise of Nasal Decolonization
Over the past decade, nasal decolonization has evolved from a targeted intervention to a standard component of infection prevention protocols.
Leading organizations in Perioperative Care and Infection Prevention recommend nasal decolonization as part of a bundled approach to reducing surgical site infections and other HAIs.3-5 This is especially relevant in:
- Orthopedic and cardiac surgeries
- ICU and long-term acute care (LTAC) settings
- High-risk or immunocompromised patient populations
Clinical evidence reinforces this shift:
- A prospective study Polley et al. with preoperative alcohol-based nasal antisepsis6
- In a real-world inpatient setting, Walker et al. reported a 63% reduction in positive cultures following implementation of a nasal decolonization protocol7
These findings highlight a key reality: reducing nasal bioburden directly impacts infection risk.
Rethinking the Nose: Nasal Decolonization Is Skin Antisepsis
One of the most important—and often misunderstood—concepts is this:
Nasal decolonization is fundamentally a form of skin antisepsis.
The nasal vestibule is lined with keratinized squamous epithelium, biologically similar to external skin—not mucosa. This distinction is critical because it changes how decolonization should be approached.
In surgical practice, skin antisepsis follows well-established principles:
- Mechanical cleaning before antisepsis
- Broad-spectrum antimicrobial application
- Defined contact time and technique
Historically, nasal decolonization has not always adhered to these same rigorously defined steps, leading to variability in outcomes.
Limitations of Traditional Approaches
Traditional nasal decolonization strategies have generally fallen into two categories:
- Topical Antibiotics (e.g., mupirocin)
- Requires multi-day patient compliance
- Increasing concerns regarding antibiotic resistance
- Operational challenges in perioperative workflows
- Single-Step Antiseptics
- Often lack mechanical cleaning, leaving organic material behind
- May not achieve consistent contact with target tissue
- Application technique can vary widely across users
These limitations point to a critical insight: Effectiveness depends not only on the agent used, but on how it is applied.
The Future of Infection Prevention Starts at the Source
As healthcare systems continue to prioritize measurable reductions in HAIs and SSIs, nasal decolonization has become a frontline preventive strategy.
However, to maximize its impact, protocols must evolve to reflect established principles of surgical skin preparation:
- Proper technique is essential
- Standardization improves outcomes
- The nasal vestibule should be treated as skin, not an exception
In a future post, we will delve deeper into how newer approaches are addressing these gaps and redefining what effective nasal decolonization looks like in clinical practice.
Eloquest Healthcare is proud to support infection prevention efforts that help translate evidence into safer clinical practice. Subscribe to receive updates on clinical insights.
For general inquiries or additional information, contact us or call 1-877-433-7626.
References:
- Centers for Disease Control and Prevention. Strategies to Prevent Hospital-Onset Staphylococcus aureus Bloodstream Infections in Acute Care Facilities. 2020.
- Bode LGM, Kluytmans JAJW, Wertheim HFL, et al. Preventing surgical-site infections in nasal carriers of Staphylococcus aureus. New England Journal of Medicine. 2010;362:9–17.
- Centers for Disease Control and Prevention. Guideline for the Prevention of Surgical Site Infection. 2017
- Society for Healthcare Epidemiology of America; Infectious Diseases Society of America. Strategies to Prevent Surgical Site Infections in Acute Care Hospitals: 2022 Update.
- Association of periOperative Registered Nurses. Guidelines for Perioperative Practice. Latest edition.
- Polley DS, et al. Evaluation of alcohol-based nasal antisepsis in surgical patients. International Journal of Surgery and Invasive Procedures. 2024, 7(2): 277-279.
- Walker K, et al. Impact of nasal decolonization protocol on infection outcomes in LTAC setting. Journal of Infectious Diseases & Therapy. 2024, 12:5.