Guidelines for Dressing Wear Time and Maintenance
Guidelines for vascular access dressings focus on improving both wear time and dressing integrity. Maintaining intact dressings is important for preventing infection and minimizing risk of skin injury. It can also reduce unnecessary dressing changes and help wear time more closely match standard parameters. According to the 2021 Infusion Therapy Standards of Practice (the Standards), transparent semipermeable membrane (TSM) dressings should be changed at least every 7 days, except for neonatal patients. However, if the dressing is compromised, it should be replaced immediately.¹
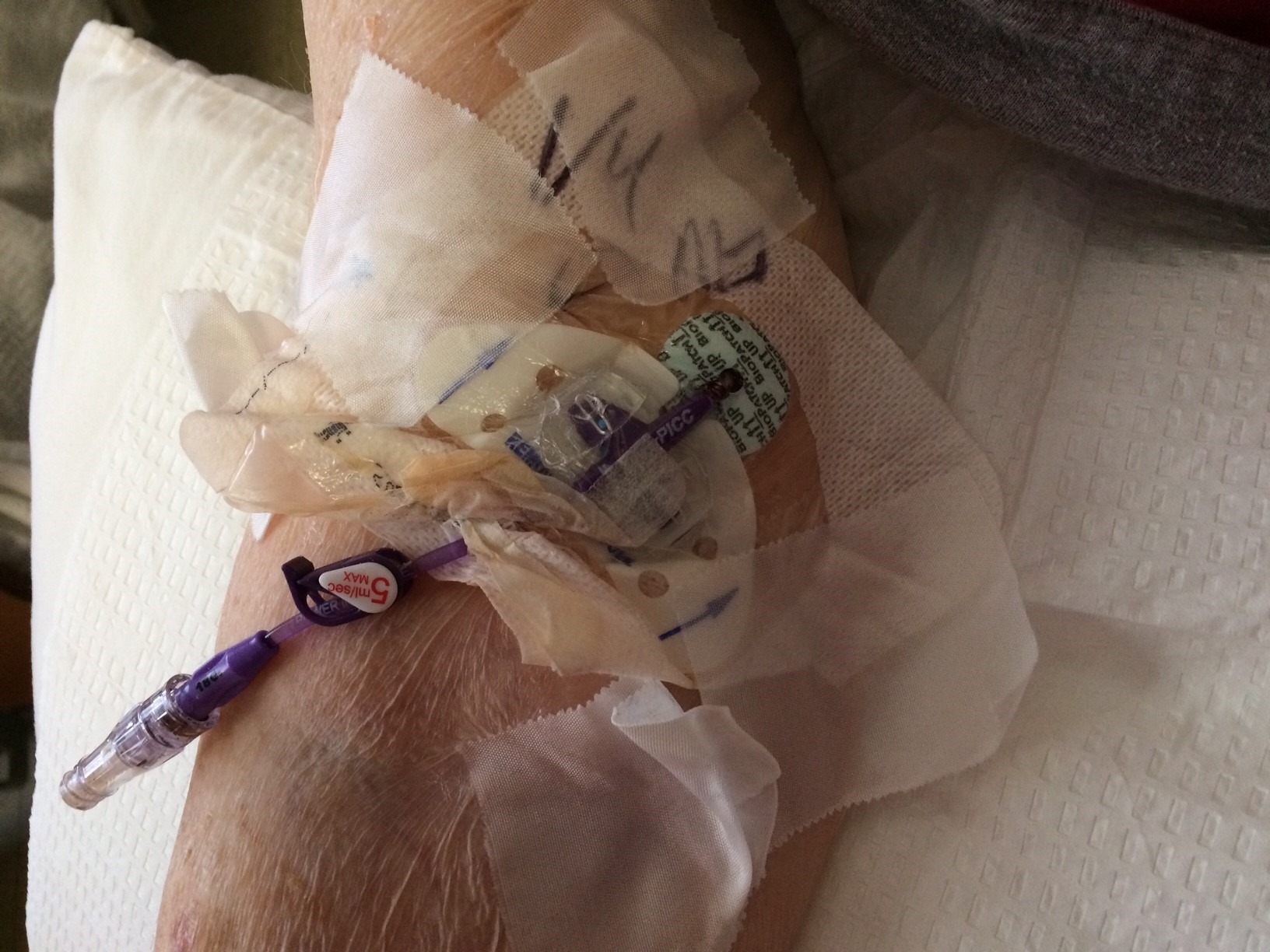
A dressing is compromised when:¹
- The border edge or transparent portion of dressing is lifted/detached
- It is visibly soiled
- Moisture, blood, or drainage is present
- Compromised skin integrity is assessed beneath the dressing
Dressing disruption is a common cause of compromised dressing integrity, which often results in early dressing replacement.² Making sure dressings are properly adhered is essential to increasing wear time and preventing complications. Not only is inadequate adherence a major cause of dressing replacement, but improved dressing adherence may lower risk of infection.³ The 2021 Standards recommend healthcare providers evaluate the beneficial use of gum mastic liquid adhesive on adult patients when enhanced dressing adherence is needed.¹
Eloquest Healthcare offers Mastisol Liquid Adhesive, a gum mastic liquid adhesive used to secure dressings, tapes, and certain medical devices over an extended period of time. To improve adherence and wear time of vascular access dressings, request a trial of Mastisol here.
Early Dressing Disruption: Frequency and Infection Risk
While dressings may be changed in response to site infection, the irony is that dressing disruption itself increases infection risk. In fact, more than 2 dressing disruptions increases risk of catheter-related infections 3-fold and infection risk grows with each additional disruption. Final dressing disruption increases odds of catheter-related infection development by 12-fold. With up to 67% of dressings being changed prematurely, this issue affects a significant portion of vascular access patients.²
Dressings may also be replaced for a variety of reasons including insufficient adherence and limited durability. A study conducted by Richardson et. al found that 4 commercially available CVC dressings had surprisingly limited wear time duration. The best performing dressing failed in under 72 hours, with 75% of evaluated CVC dressings lasting less than 48 hours. Only 3% of the tested dressings lasted the full 7 days recommended by the 2021 Standards. That means that 97% of evaluated dressings failed to meet standard wear time guidelines by a significant margin.³
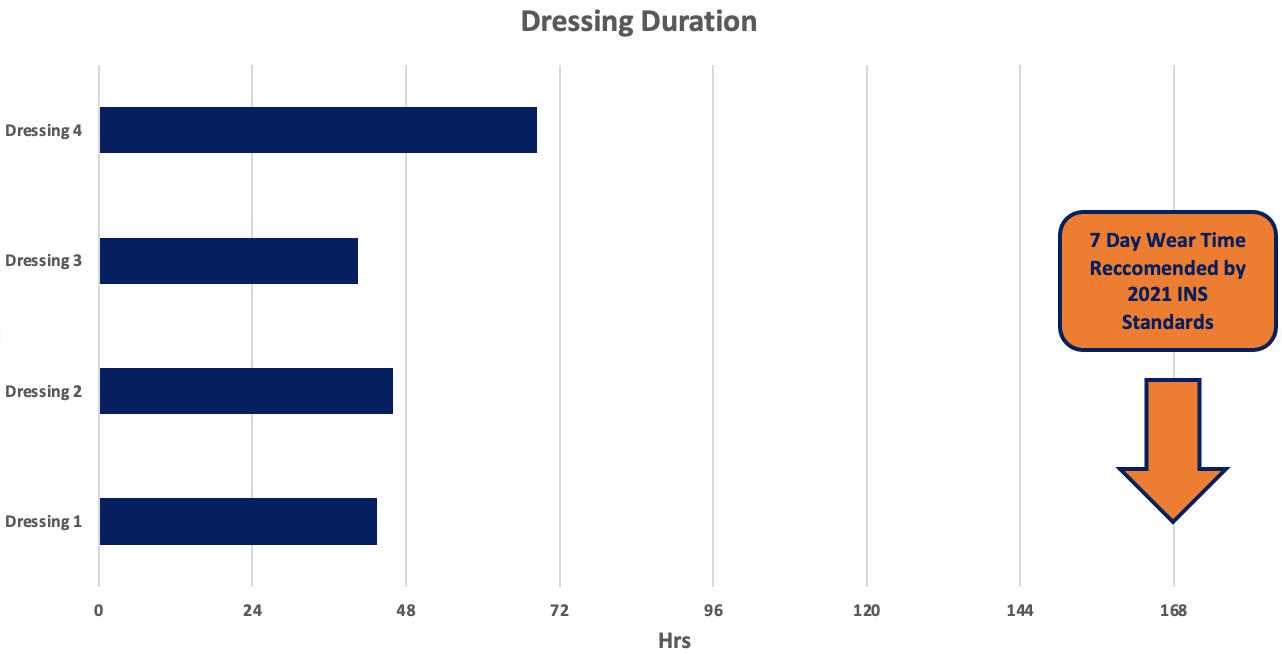
Graphic created with data from Richardson, et. al.
Addressing the Gap between Guidelines and Adherence
As seen here, there is a clear gap between dressing wear time guidelines and average dressing performance and practices.³ Healthcare organizations are actively addressing this disparity and striving to meet evidence-based guidelines to improve patient health and quality of care. This can be achieved through a combination of consistent, thorough site assessment, monitoring dressing durability, and application of gum mastic adhesive when needed. ¹,³
Eloquest Healthcare, Inc. can partner with your institution to facilitate a Vascular Access Device Site Assessment to determine the state of both dressing and skin integrity for patients in your facility, while providing you and your team with information on your facility’s infection risk, nurse efficiency, and product waste. Click here to request a Vascular Access Device Site Assessment today!
Would you like to learn more about developing an effective vascular access strategy to highlight issues that improve patient outcomes and reduce costs for your organization? Join us for a complimentary, three-part webinar series on the Vascular Access Jamboree: A ‘How To’ Guide. Everything you need to know to create a successful jamboree! Watch On Demand here.

References
- Infusion Therapy Standards of Practice: Vascular Access Device Assessment, Care, and Dressing Changes. J Infus Nurs. 2021;44:S119-S123
- Timist J-F, et al. Dressing disruption is a major risk factor for catheter-related infections. Crit Care Med. 2012;40(6):707-14.
- Richardson A, Melling A, Straughan C. Central venous catheter dressing durability: an evaluation. J Infect Prev. 2015;16:256-61.