The newly released 2021 Infusion Therapy Standards of Practice (the Standards) has been substantially updated from the previous edition. Continuing to improve and standardize practice based on evidence improves patient quality of care and boosts efficiency at the same time. The Standards are rich with many new or refined practice recommendations, based on the ever-evolving body of clinical evidence. The focus of the article are key changes in the Standards related to: Vascular Access Device Care & Dressing Changes (Standard 42) and Catheter-Associated Skin Injury (Standard 55).

What is a Compromised Dressing?
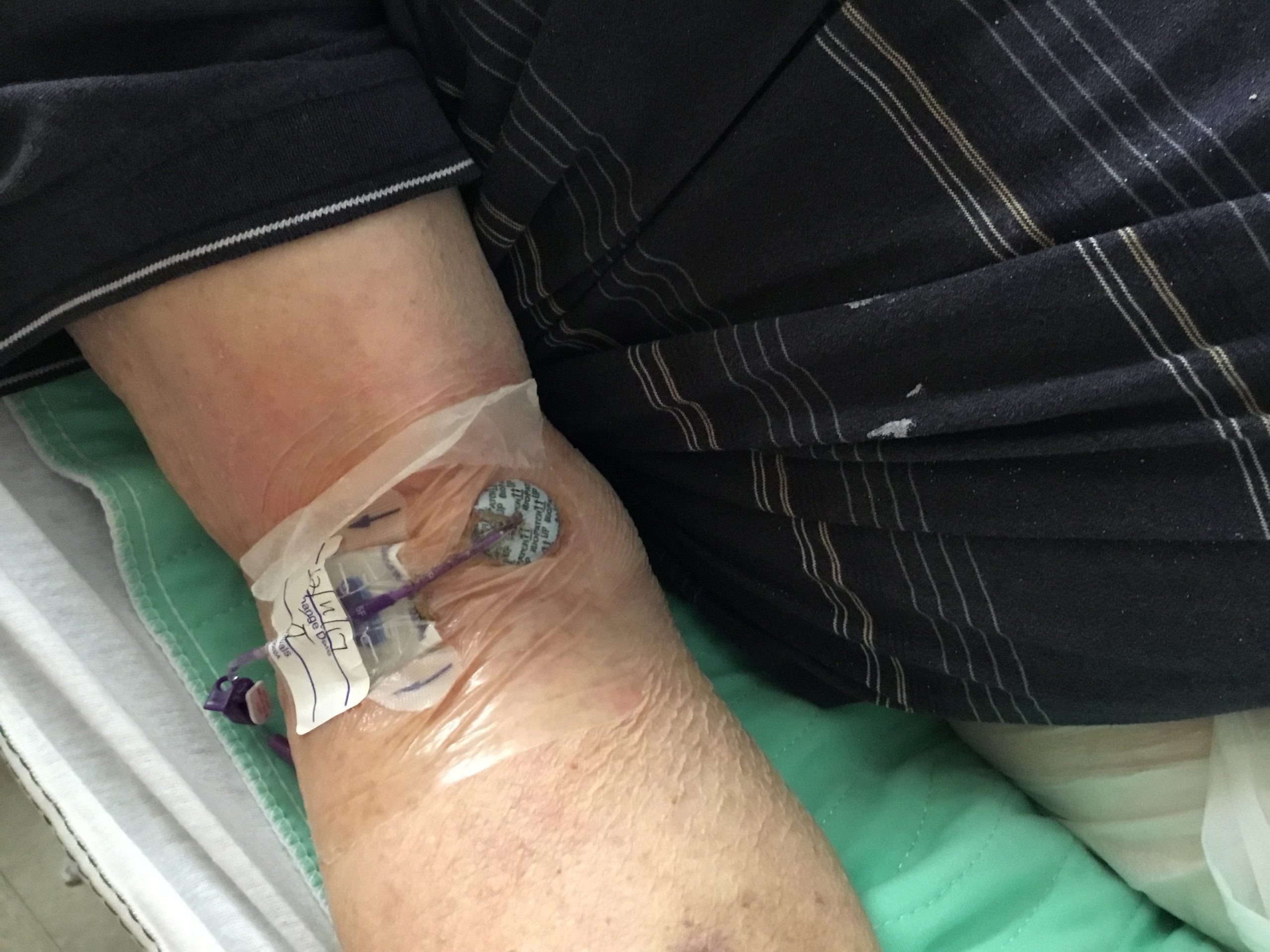
Improper adhesive practices compromise dressing integrity and can lead to the development of health care-associated infections (HAIs).1 Making sure dressings are maintained by following clear, standard guidelines is key to preventing these infections. An important, corresponding revision in the 2021 Standards is a more precise definition of “loosened” dressings, which helps healthcare providers recognize when a dressing is not intact. Previously, defining what constituted a “loose” dressing had been a common question among healthcare providers.
The 2021 Standards resolve this issue by including a more precise definition: identifying a loose dressing as “lifted/detached on any border edge or within transparent portion of dressing.”2 This further standardization of dressing site care and maintenance continues to prioritize patient well-being.
Other signs a dressing may be compromised include whether it is visibly soiled, skin impairment is evident, or if there is significant moisture, drainage, or blood. The 2021 Standards emphasize the importance of changing dressings immediately if they have been disrupted. However, if the dressing remains intact, the recommendation has been updated to changing transparent semipermeable membrane (TSM) dressings at least once every 7 days.2 Previously, the guidelines had been to change such dressings at least every 5-7 days.3
Specific Practice Recommendations for Use of Gum Mastic Adhesive
Securing dressings effectively is a necessary step during application, since multiple dressing changes due to material disruption or dislodgement are associated with greater risk of catheter-related bloodstream infections (CRBSI).1 While the previous edition of the Standards included the importance of securing dressings, no advice on how to do so was provided. Recommendations now specify to evaluate the benefits of gum mastic liquid adhesive in order to better ensure dressings remain intact.2
Notable Terminology Updates
A vocabulary update has introduced the term “Catheter-Associated Bloodstream Infection” (CABSI) to encompass all bloodstream infections (BSIs) stemming from peripheral intravenous catheters (PIVCs) or central vascular access devices (CVADs). Previously, terms including catheter-related bloodstream infection (CRBSI) and central line-associated bloodstream infection (CLABSI) were used.2 The broader acronym CABSI serves to reduce confusion and further standardize diagnosis and treatment.
Another significant update was included in the newly released Standards. A new Standard was added: Catheter-Associated Skin Injury. Catheter-associated skin injury can happen when securement devices are changed, with likelihood of occurrence increasing with age, joint movement, and presence of edema. It is essential that Vascular Access Device (VAD) sites are closely monitored for signs of skin injury.2
Removal of Adhesive to Prevent Injury & Infection
Proper removal of adhesive materials is essential to prevent infection and skin irritation/damage that may occur due to adhesive residue. The Standards state that healthcare providers should make sure all residual adhesive is removed from the skin during antisepsis processes.2
Standardized Dressing Kits
Using pre-packaged dressing kits to further standardize patient care is also recommended in the Standards.2 Having every critical item for dressing changes in one kit ensures all patients receive the same level of care, while also boosting efficiency.
Protocol Changes Necessitate Audit and Feedback
The 2021 Standards recommends using audit and feedback to implement protocol changes in vascular device/dressing care and maintenance. Strict, detailed monitoring of skin condition, especially catheter-associated skin injuries, is also highly recommended.2
Eloquest Healthcare can help your team achieve this practice recommendation by providing resources to facilitate observational data collection on rates of dressing adherence, skin condition, and compliance with guidelines. This is completed through a Vascular Access Dressing Point Prevalence Assessment. Partnering facilities are provided a comprehensive report of the VAD site observations organized by infection risk, nurse efficiency, and financial analysis. For more information on Point Prevalence assessments, contact your sales consultant or Eloquest Healthcare®, Inc., at 1‐877‐433‐7626 or schedule a Point Prevalence assessment for your facility here.
Eloquest Healthcare offers Mastisol®, a gum mastic liquid adhesive, used to secure dressings, tapes, and certain medical devices thereby minimizing risk of infection. Its use is supported by evidence-based best practice guidelines. Eloquest also offers Detachol® Adhesive Remover, a non-irritating adhesive remover in an easy-to-use sterile applicator. It minimizes risk of discomfort and skin injury associated with removal of dressings, tapes, and sticky residue from the skin.
Updates in the 2021 Standards continue to emphasize standardization of dressing care and maintenance in an effort to ensure that all patients receive quality care. Sharing that same goal, Eloquest Healthcare’s products and initiatives support strategies that prevent hospital acquired infections and provide better outcomes, higher quality and lower healthcare costs.
For more information about Mastisol® Liquid Adhesive or Detachol® Adhesive Remover, please contact your sales consultant or Eloquest Healthcare®, Inc. Call 1‐877‐433‐7626 or fill out this form.

References
- Timsit, JF, Bouadma L, Ruckly S, Schwebel C, Garrouste-Orgeas M, Bronchard R, Calvino-Gunther S, Laupland K, Adrie C, Thuong M, Herault MC, Pease S, Arrault X, Lucet JC. Dressing disruption is a major risk factor for catheter-related infections. Crit Care Med. 2012;40:1707-14.
- Gorski, LA, Hadaway, L, Hagle, ME, et al. Infusion Therapy Standards of Practice. 8TH J Infus Nurs. Revised 2021.
- Gorski L.A., Hadaway L., Hagle M., McGoldrick M., Orr M., Doellman D. 2016 Infusion therapy standards of practice. Journal of Infusion Nursing. 2016;39:S1–
S159.